Ocular Risk Factors Affecting Intraoperative Complications In Mature Cataract Surgery
Doi: 10.36351/pjo.v41i2.1970
DOI:
https://doi.org/10.36351/pjo.v41i2.1970Abstract
Purpose: To identify the demographic and ocular risk factors associated with complications in phacoemulsification and planned extracapsular cataract extraction (PECCE) for mature cataracts.
Study Design: Retrospective chart analysis.
Place and Duration of Study: Haydarpaşa Numune Training and Research Hospitalfrom January 2018 and December 2021.
Methods: A total of 236 eyes of 236 patients who underwent surgery for mature cataracts between 2018 and 2021 were included in the study. Demographic characteristics, presence of pseudoexfoliation, cataract type, pupil dilation, anterior chamber depth, presence of phacodonesis, preoperative best-corrected visual acuity, intraocular pressure, intraoperative and postoperative surgical complications, and postoperative first month visual acuity were analyzed.
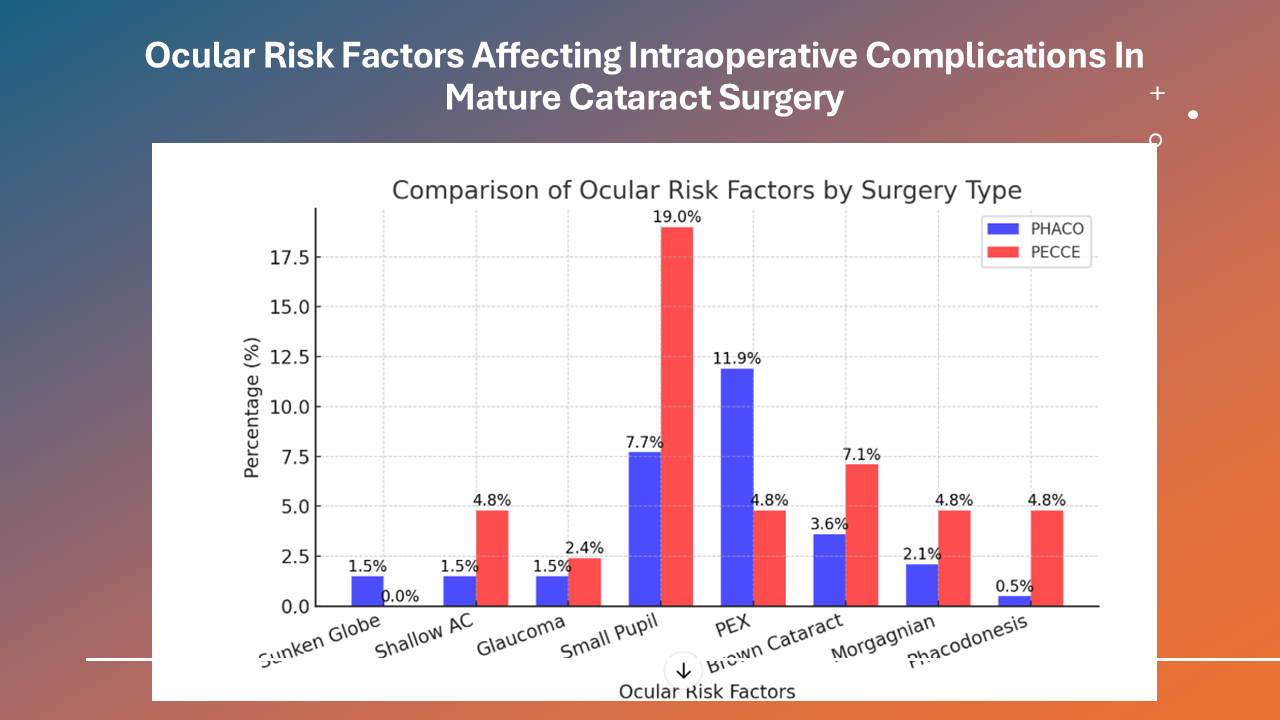
Results: A total of 194 eyes (82%) underwent phacoemulsification, while 42 eyes (18%) underwent PECCE. The mean age and mean preoperative BCVA LogMAR values were significantly higher in the PECCE group (p=0.001 and p=0.027, respectively). Among ocular risk factors, only pupillary mid-dilation was significantly higher in the PECCE group (p=0.04). Intraoperative complications were more frequent in brown cataracts within the PHACO group compared to eyes without brown cataracts (p=0.004). Additionally, intraoperative complications, postoperative complications, and the need for postoperative revision were significantly higher in the PECCE group (p<0.05 for all).
Conclusion: The preoperative rate of mid-dilated pupils was higher, and preoperative visual acuity was lower in eyes with mature cataracts undergoing PECCE surgery. The presence of brown cataracts was associated with an increased risk of complications in PHACO surgery.
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2025 Doğukan Cömerter, Yasemin Un, Okşan Alpoğan, Melike Sarıdoğan

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.









